When natural conception does not occur as expected, couples are often advised to consider assisted reproductive treatments. The two most common first-line options are IUI (Intrauterine Insemination) and IVF (In Vitro Fertilization).
While both aim to increase the probability of pregnancy, they differ significantly in complexity, cost, indications, and success rates. Choosing the right treatment depends on age, diagnosis, duration of infertility, and prior treatment history.
This article offers a structured comparison to help couples make informed decisions.
What Is IUI?
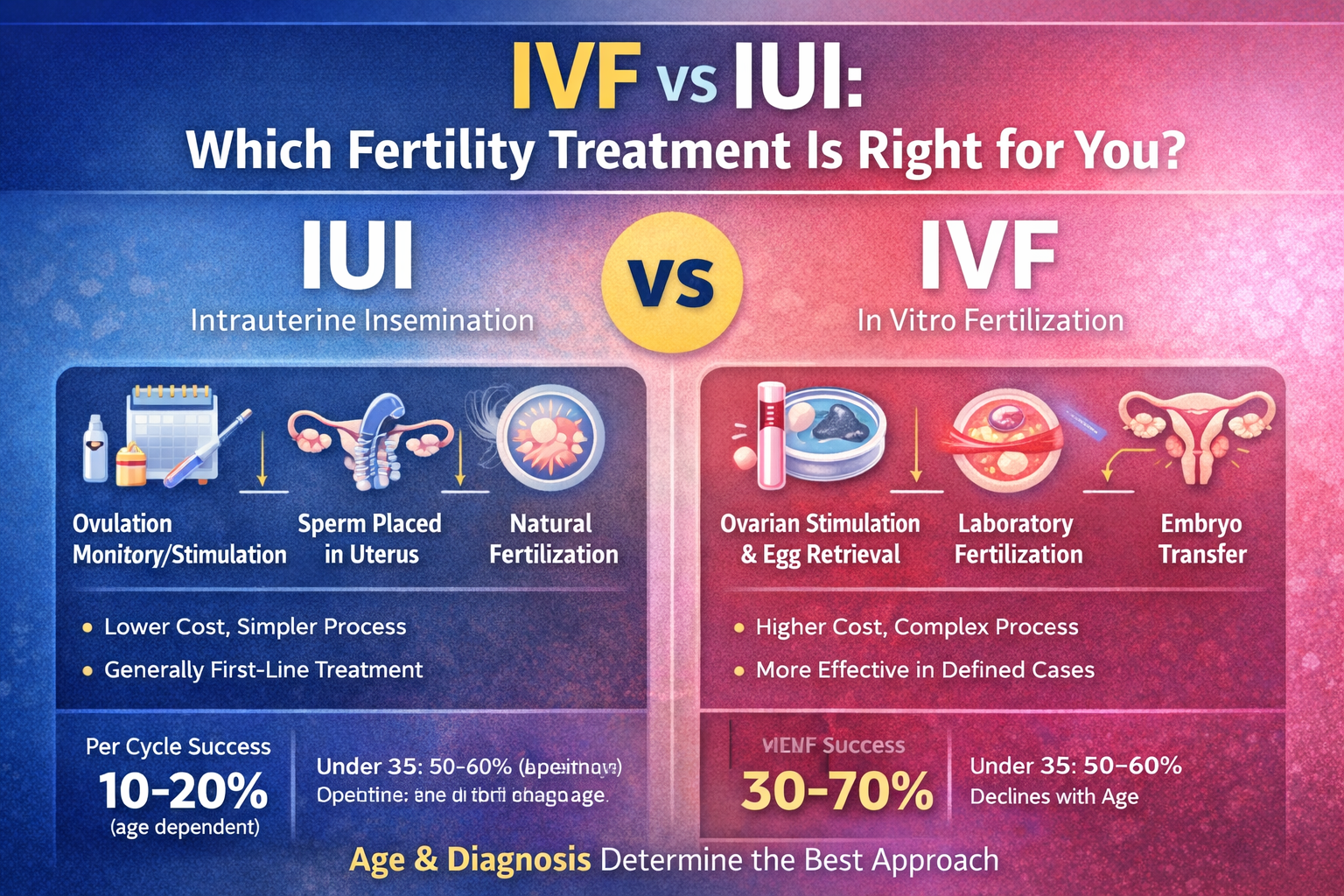
IUI is a relatively simple fertility procedure in which:
- Ovulation is monitored or medically stimulated
- Processed (washed) sperm is placed directly inside the uterus
- Fertilization occurs naturally inside the body
For couples seeking IUI Treatment in Chandigarh, this procedure is often recommended as the first step when infertility issues are mild and the ovarian reserve is good.
What Is IVF?
IVF is an advanced assisted reproductive technique involving:
- Ovarian stimulation to produce multiple eggs
- Egg retrieval under ultrasound guidance
- Laboratory fertilization (IVF or ICSI)
- Embryo culture
- Embryo transfer into the uterus
Fertilization occurs outside the body in a controlled laboratory setting. At specialized centers like Reviva IVF, advanced laboratory protocols help improve embryo quality and pregnancy outcomes.
Indications: When Is IUI Recommended?
IUI is generally suitable when:
- Mild male factor infertility
- Unexplained infertility
- Mild ovulatory dysfunction
- Cervical factor infertility
- Short duration of infertility
- Woman is under 35 with good ovarian reserve
It is often recommended for 3–4 cycles before considering escalation.
Indications: When Is IVF Recommended?
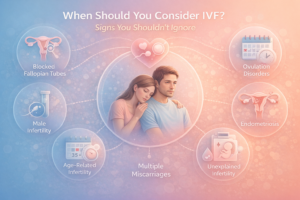
IVF is typically advised when:
- Blocked or damaged fallopian tubes
- Moderate to severe male factor infertility
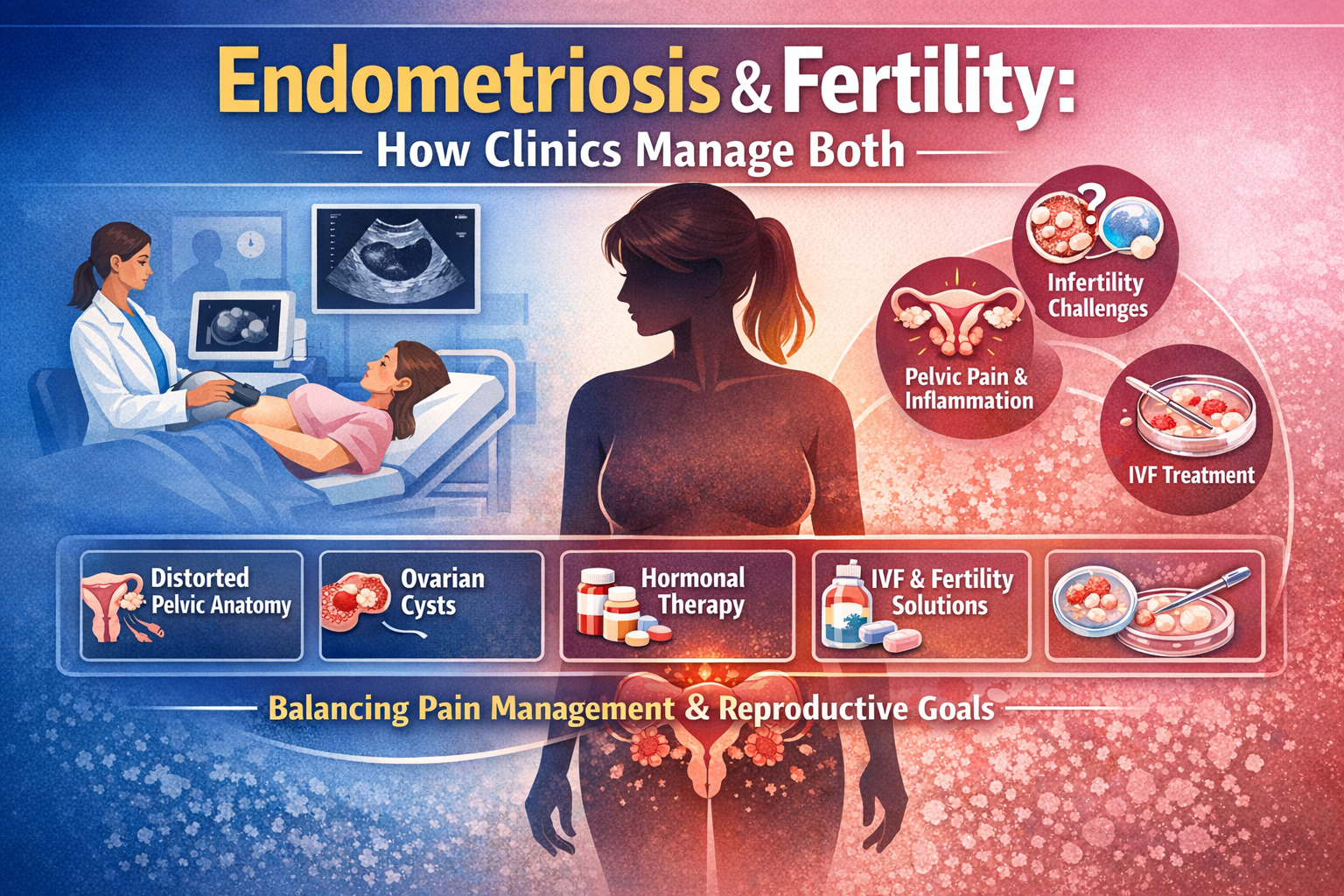
- Endometriosis (moderate to severe)
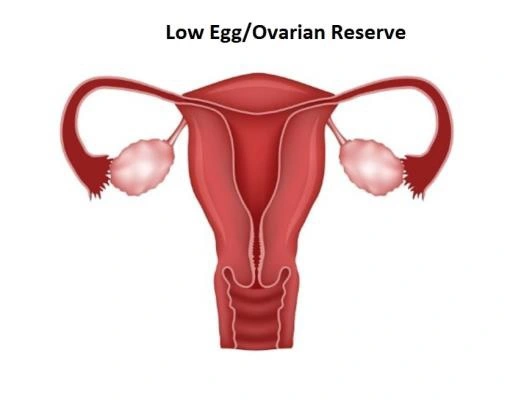
- Low ovarian reserve
- Repeated IUI failures
- Age above 35 with limited time
- Genetic testing requirement
In such cases, treatment at a Best IVF Centre significantly improves the chances of conception.
Success Rate Comparison
IUI Success Rate
- Per cycle success: 10–20% (age dependent)
- Higher success in women under 35
- Declines sharply after 37
Cumulative success improves over multiple cycles but remains lower than IVF.
IVF Success Rate
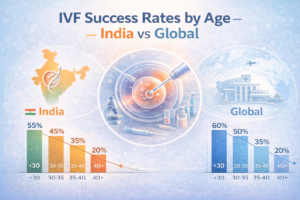
- Under 35 years: 50–60% per cycle
- 35–37 years: 35–45%
- 38–40 years: 20–30%
- Above 40 years: 5–15% (using own eggs)
IVF provides substantially higher pregnancy rates, especially in defined medical conditions.
Cost Considerations
- IUI is significantly less expensive per cycle.
- IVF costs more per attempt but offers higher per-cycle success.
In some cases, repeated IUI failures may ultimately cost more emotionally and financially than earlier IVF.
Strategic planning based on diagnosis is essential.
Time Sensitivity & Age Factor
Age is a decisive variable.
- Women under 30 with mild issues may reasonably attempt IUI first.
- Women above 35 often benefit from early IVF to maximize reproductive potential.
- Women above 38 may lose valuable time attempting multiple IUIs with limited probability.
Delays can reduce cumulative success.
Emotional and Physical Burden
IUI:
- Less invasive
- Minimal discomfort
- Lower medication dosage
- Shorter treatment cycle
IVF:
- Requires injections
- Egg retrieval procedure
- Emotional investment per cycle
- Higher psychological intensity
However, IVF may shorten the overall treatment journey by achieving pregnancy faster.
Risk Profile
IUI Risks:
- Multiple pregnancy (if stimulation is aggressive)
- Low complication rate
IVF Risks:
- Ovarian Hyperstimulation Syndrome (OHSS)
- Multiple pregnancy (controlled through single embryo transfer)
- Procedure-related minor risks
Modern protocols have significantly improved safety.
Diagnostic-Based Decision Framework
A simplified clinical perspective:
- Mild infertility + young age → Consider IUI
- Tubal blockage → IVF mandatory
- Severe male factor → IVF with ICSI
- Endometriosis (Stage III/IV) → IVF preferred
- Repeated IUI failure → Escalate to IVF
- Advanced maternal age → IVF recommended
Individualization is critical—there is no universal formula.
Psychological Perspective
Couples often prefer starting with IUI due to:
- Lower cost
- Perception of being “less intense”
- Emotional readiness
However, realistic counseling helps prevent prolonged, ineffective treatment cycles.
The goal is not the simplest treatment—it is the most effective treatment for your specific diagnosis.
Key Takeaways
- IUI is simpler and affordable but has lower per-cycle success.
- IVF is more advanced and costly but significantly more effective in defined cases.
- Age and diagnosis should guide the decision—not just cost.
- Delayed escalation may reduce overall success probability.
- A structured fertility evaluation ensures optimal treatment sequencing.