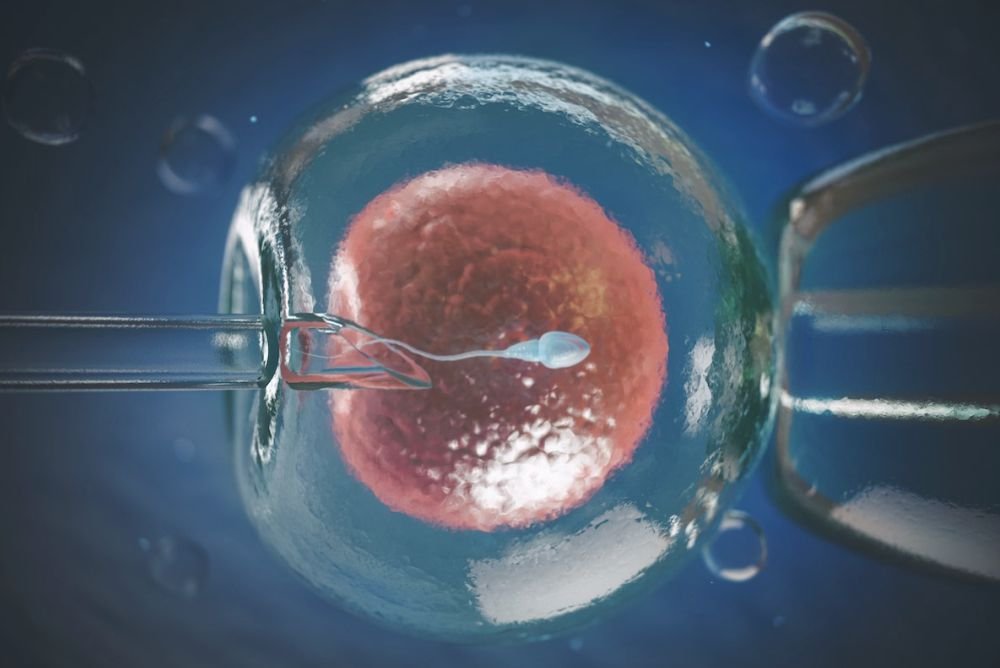
When an embryo fails to implant despite being of good quality, the cause often lies not in the embryo itself, but in the uterine lining—specifically, its ability to receive and nurture the embryo. This ability, known as endometrial receptivity, is one of the most crucial and least understood factors in IVF success.
At Reviva IVF, Chandigarh, our specialists focus not just on creating strong embryos but on ensuring that the uterus is perfectly synchronized to accept them. Through advanced diagnostic tools like ERA (Endometrial Receptivity Analysis), we customize embryo transfer timing for each patient, improving the chances of a healthy pregnancy.
What Is Endometrial Receptivity?
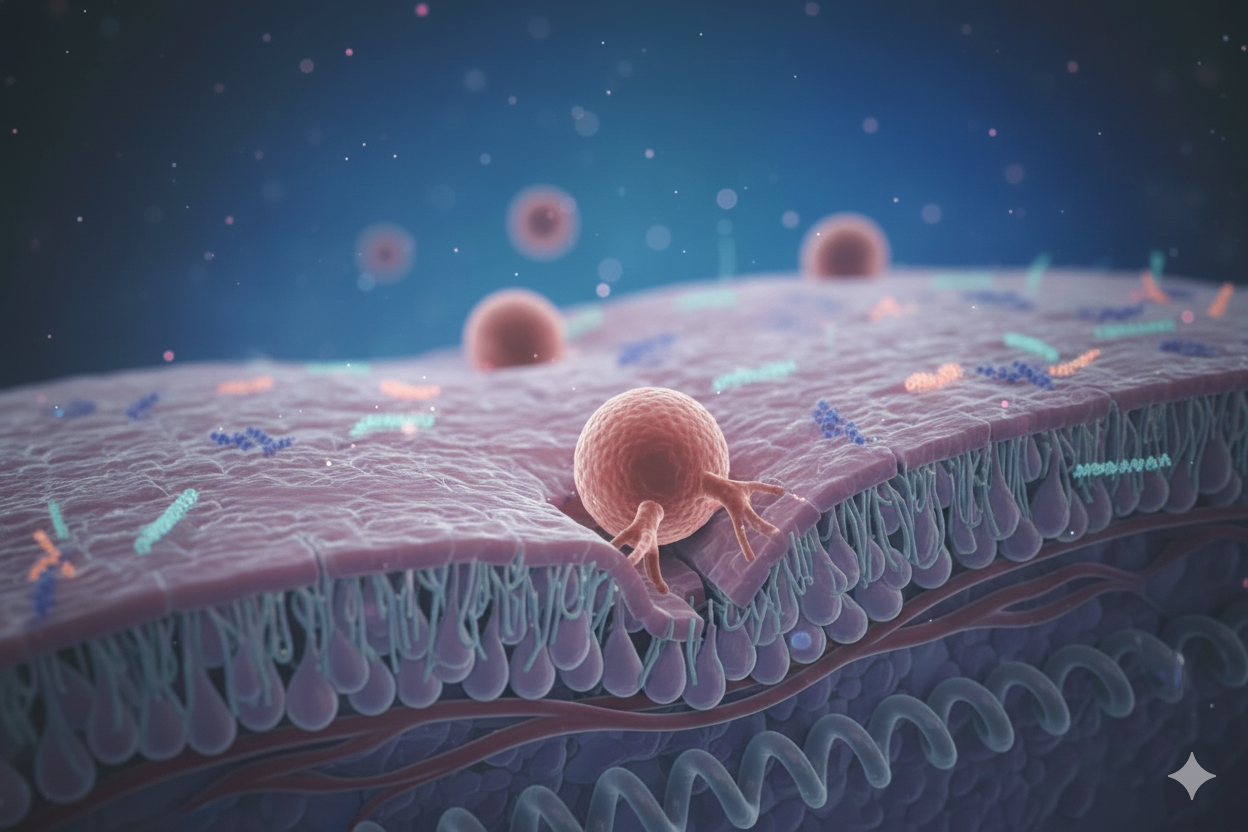
The endometrium (uterine lining) undergoes cyclic changes under the influence of estrogen and progesterone. There is a short period—usually between Day 19 and Day 23 of a regular cycle—when it is most receptive to an embryo. This is called the “Window of Implantation.”
If the embryo is transferred outside this window, implantation may fail even if both the embryo and uterus are otherwise healthy.
“Even the best embryo needs the right moment to meet its home.” — Dr. Deepika Gupta, Senior Fertility Specialist, Reviva IVF
Why Endometrial Receptivity Matters
A receptive endometrium allows the embryo to attach, invade, and form a healthy placenta. When receptivity is poor, issues like implantation failure, early miscarriage, or thin endometrium may occur.
Common causes include:
- Hormonal imbalance or luteal phase defect.
- Excess estrogen or insufficient progesterone.
- Chronic endometritis or infection.
- Thin endometrial lining (<7mm).
- Autoimmune and inflammatory conditions.
How Reviva IVF Assesses Endometrial Receptivity
- Ultrasound and Doppler Assessment
– Measures endometrial thickness, pattern, and blood flow. - Hormonal Evaluation
– Ensures adequate progesterone and estrogen levels before embryo transfer. - Endometrial Receptivity Analysis (ERA Test)
– A molecular diagnostic test that evaluates the expression of over 200 genes linked to receptivity.
– Determines whether the “window of implantation” is normal, delayed, or advanced.
With ERA, Reviva IVF creates a Personalized Embryo Transfer (pET) plan that aligns embryo transfer timing with the patient’s unique biological clock.
Optimizing the Uterine Environment
Beyond diagnostics, Reviva IVF employs multiple therapies to improve endometrial health:
- PRP (Platelet-Rich Plasma) Therapy to stimulate endometrial growth.
- G-CSF Infusion for thin lining cases.
- Luteal-phase support with progesterone supplementation.
- Lifestyle and dietary interventions to enhance uterine blood flow.
“Endometrial receptivity isn’t just about measurement—it’s about creating the perfect microenvironment for life to begin.” — Reviva IVF Embryology Team
When to Consider ERA Testing
- Repeated IVF failures despite good-quality embryos.
- Unexplained implantation failure.
- Women above 37 years.
- Patients with irregular menstrual cycles or hormonal imbalance.
- History of thin endometrium or poor response to progesterone.
ERA-guided embryo transfers have shown 20–25% higher implantation rates compared to conventional timing, especially in recurrent failure cases.
The Reviva IVF Difference
- Advanced molecular diagnostics for ERA and hormone mapping.
- Expertise in synchronized, personalized embryo transfer.
- Integration of endometrial therapies into IVF protocols.
- Comprehensive follow-up to monitor uterine health post-transfer.
Conclusion
Endometrial receptivity is the bridge between science and nature—where precision meets timing.
At Reviva IVF, Chandigarh, our approach ensures that every transfer happens at the most receptive moment, giving every embryo the best possible chance to implant and grow.
Because success in IVF isn’t just about creating life—it’s about preparing the perfect place for it to begin.