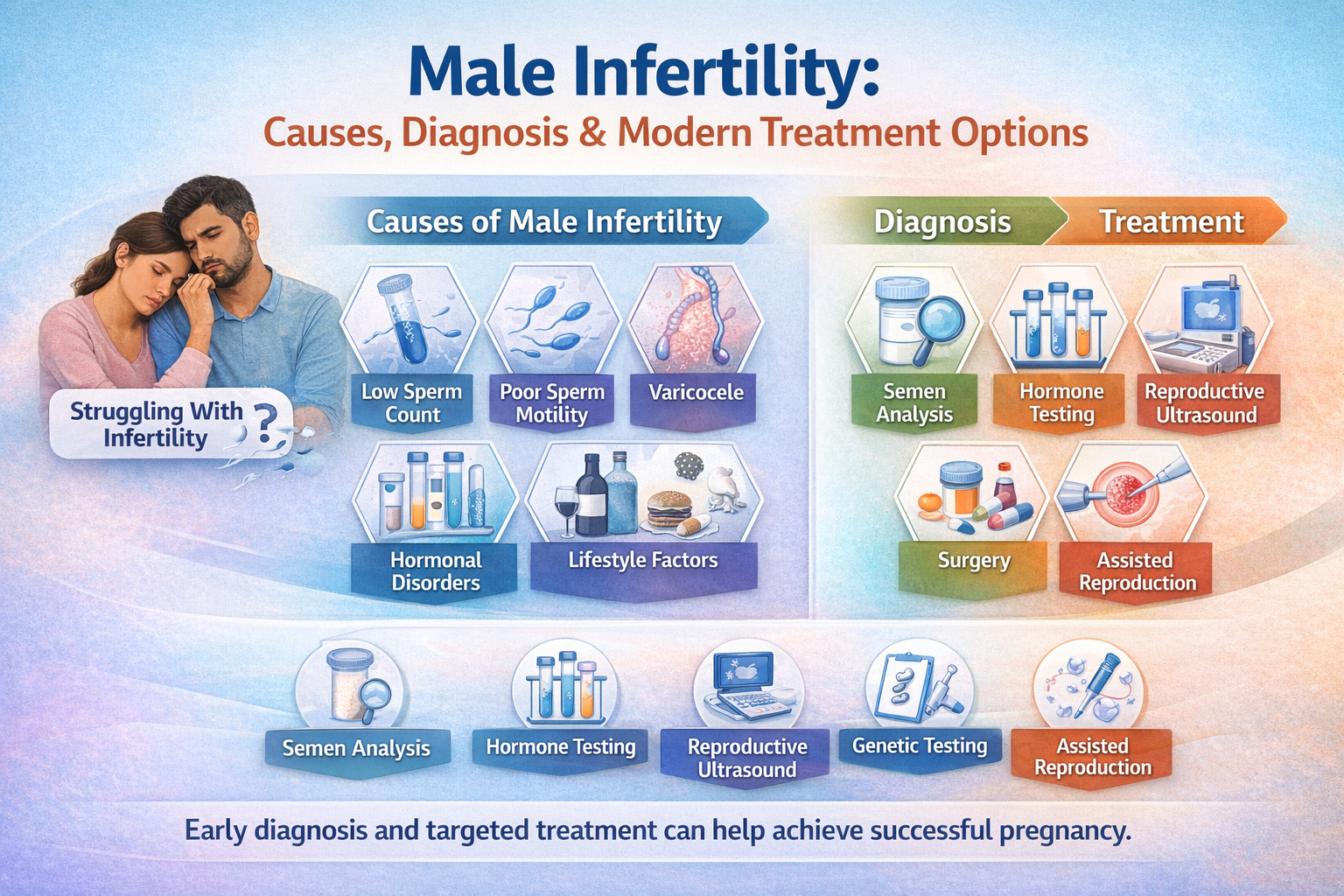
Infertility affects millions of couples worldwide, and in nearly 40–50% of cases, male factors contribute to the problem. Understanding male infertility is essential for early diagnosis and effective treatment.
What is Male Infertility?
Male infertility occurs when a man has difficulty causing pregnancy due to problems related to sperm production, sperm function, or sperm delivery.
Common symptoms may include:
- Low sperm count
- Poor sperm motility
- Abnormal sperm shape
- Hormonal imbalances
Often, male infertility does not show obvious symptoms and is diagnosed only after medical testing.
Common Causes of Male Infertility
1. Low Sperm Production
Some men produce fewer sperm than normal, reducing the chances of fertilization.
2. Poor Sperm Motility
Motility refers to the ability of sperm to swim effectively toward the egg.
3. Varicocele
Varicocele is an enlargement of veins in the scrotum that can affect sperm quality.
4. Hormonal Disorders
Hormones play an essential role in sperm production. Imbalances can lead to infertility.
5. Lifestyle Factors
Certain lifestyle habits may reduce sperm health, including:
- Smoking
- Excess alcohol
- Obesity
- Stress
- Poor diet
6. Medical Conditions
Infections, genetic disorders, or previous surgeries may also affect fertility.
How Male Infertility is Diagnosed
Diagnosis usually begins with a semen analysis, which evaluates sperm count, motility, and morphology.
Other tests may include:
- Hormone testing
- Ultrasound of reproductive organs
- Genetic testing
- Sperm DNA fragmentation test
These tests help fertility specialists determine the underlying cause.
Modern Treatment Options
Fortunately, many cases of male infertility can be treated successfully.
Lifestyle Improvements
Healthy habits can significantly improve sperm health.
- Balanced diet
- Regular exercise
- Avoiding tobacco and alcohol
- Stress management
Medications
Hormonal medications may help correct imbalances affecting sperm production.
Surgical Treatments
Procedures like varicocele repair can improve sperm quality in some cases.
Assisted Reproductive Techniques
Modern fertility treatments offer hope for couples struggling with male infertility.
IUI (Intrauterine Insemination): Processed sperm is directly placed in the uterus.
ICSI (Intracytoplasmic Sperm Injection): A single healthy sperm is injected directly into the egg.
IVF (In Vitro Fertilization): Eggs and sperm are combined in a laboratory to form embryos.
Importance of Early Evaluation
Many couples assume infertility is only related to women, but male fertility plays an equally important role. Early testing can save time and help couples choose the right treatment.
If you have been trying to conceive for more than a year without success, consulting Reviva IVF fertility specialists can help identify the cause and guide you toward effective solutions.